Maximize Your Financial Performance

Unparalleled insights and benchmarks on negotiated rates.
Contact us for a demo
CONTEXT
Starting on July 1st, 2022, based on the CMS Transparency in Coverage Final Rule, the Federal Government requires health insurers and group health plans, including self-funded clients, to publish and update on a monthly basis pricing data in "machine readable formats" for covered items and services based on in-network negotiated payment rates and historical out-of-network allowed amounts.
CHALLENGE
This newly accessible data is immense, potentially surpassing the size of the Library of Congress. Likely, the total size of the data published by the payers would be close to 1 Petabyte (which is 1,024 TB, or 1,048,576 GB).
SOLUTION
Discover PayerAnalytics: a leading-edge SaaS platform designed to distill actionable insights and benchmarks from complex reimbursement rate data, empowering both providers and plans for strategic decision-making.
SO WHAT
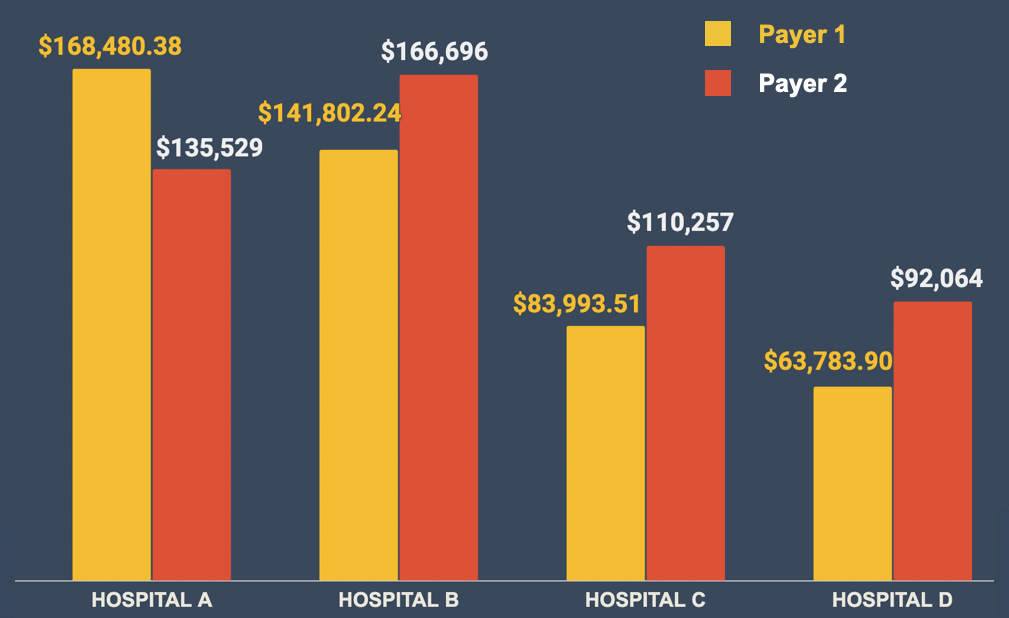
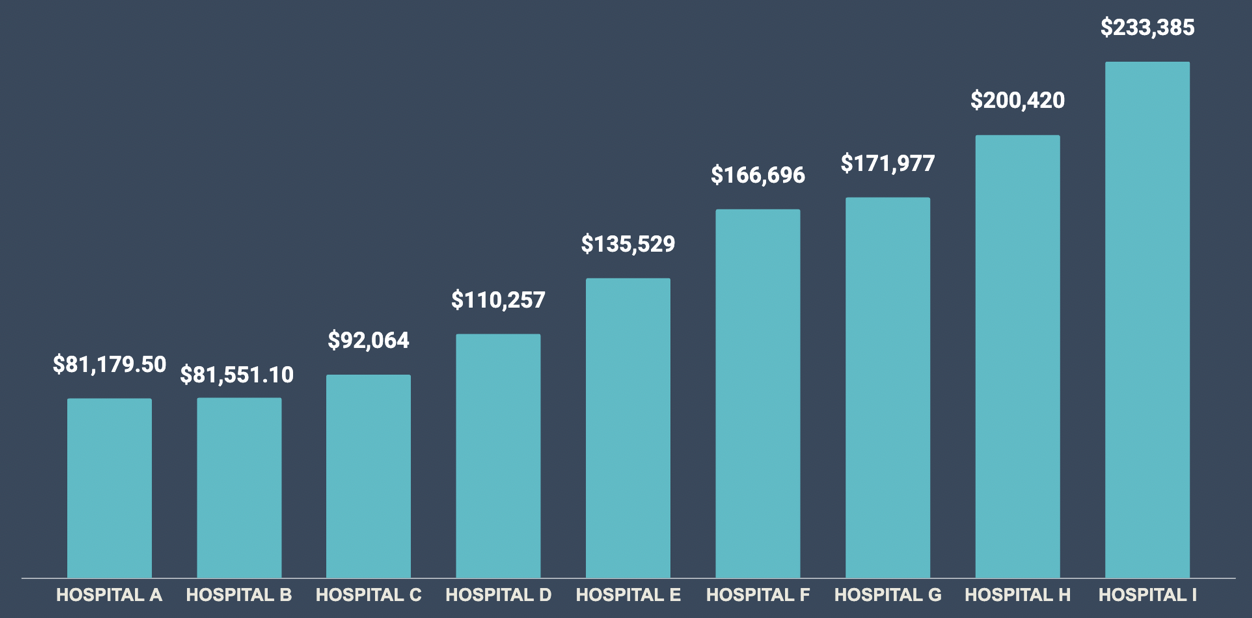
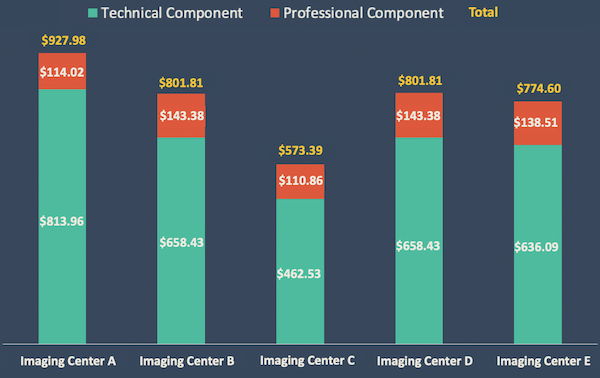
Visualize a scenario where your rates could be optimized: If you charge $500 for a clinical service while a nearby competitor charges $750, PayerAnalytics enables you to identify and adjust your rates, ensuring you're not undervaluing your services.


IDENTIFY
Optimize rates for higher reimbursements and maximizing revenue potential.

COMPARE
Benchmark your rates against the competition to identify opportunities.

GROW
Secure higher negotiated rates to increase revenue and improve margins.

COMPETE
Negotiate from a position of strength with competitive rate analytics.